What to Do to Keep Your Child’s Feet Healthy
Being a parent involves caring for your child in every way you can. You make sure they are eating the right food, being nice to others, and staying out of any trouble. However, it is also important that you are watchful of their health, more specifically their foot health. Maintaining good foot health in childhood is important in preventing later conditions in life from happening. As children continue to develop, their feet require different techniques of care. Here are some various ways in which you can help your child’s feet stay healthy.
A baby needs a lot of care and attention overall, but the importance of their feet should never be forgotten. Before a baby turns one, their feet change and develop greatly. It is important that during this time, a mother avoids putting tight socks on their child. She should also encourage movement of their feet so the baby can begin to feel more comfortable using them.
As a baby enters the toddler years of his or her life, they are begin to walk around. When your baby begins to take those first steps, it is crucial that they are wearing protective shoes on their feet. As a mother that is observant of your child’s feet, you may notice changes in them. This is completely normal as the feet are becoming susceptible to the activity of walking. It is normal for a toddler to be a bit unsteady or to “walk funny” at first.
When your child grows out of their toddler years, it is important that you begin to show him or her how to care for their feet on their own. Practice with your child proper hygiene in order to prevent foot fungus or infection. Since children are constantly on the move, it is crucial to be cautious of any accidents or injuries that might occur. If an injury occurs, it is advised that you take your child to be examined by a doctor immediately. Since your child is still growing, particular injuries can shift the way in which a bone or other important part of the foot is developing.
Babies and kids are always changing and growing. Your job as a parent is to make sure they stay healthy and making sure they are properly maintained. This involves proper foot care and making sure the feet stay healthy. Following this guide, your child can live a long and happy life.
Treatments for Corns
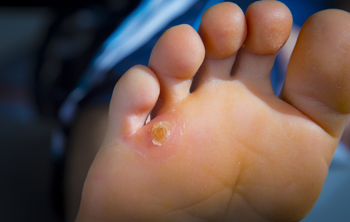 Corns are circular areas of raised, thickened skin that can usually be found on or around the toes. They are caused by repetitive friction over an area of skin. Corns can be soft or hard, depending on their location. Soft corns are more likely to form in between the toes, whereas hard corns are more likely to form on the tops or sides of toes. Corns may need medical attention if they are painful or if you have a medical condition like diabetes or a connective tissue disease. With your podiatrist’s approval, you may soak the corns in warm water and file them down with a pumice stone at home. You may also be prescribed a plaster to wear over the corn or a cream to apply to it to soften the thickened skin. For more information about corns, please consult with a podiatrist.
Corns are circular areas of raised, thickened skin that can usually be found on or around the toes. They are caused by repetitive friction over an area of skin. Corns can be soft or hard, depending on their location. Soft corns are more likely to form in between the toes, whereas hard corns are more likely to form on the tops or sides of toes. Corns may need medical attention if they are painful or if you have a medical condition like diabetes or a connective tissue disease. With your podiatrist’s approval, you may soak the corns in warm water and file them down with a pumice stone at home. You may also be prescribed a plaster to wear over the corn or a cream to apply to it to soften the thickened skin. For more information about corns, please consult with a podiatrist.
Corns can make walking very painful and should be treated immediately. If you have questions regarding your feet and ankles, contact Brian D. Jackson, DPM of Neuhaus Foot and Ankle. Our doctor will treat your foot and ankle needs.
Corns: What Are They? And How Do You Get Rid of Them?
Corns are thickened areas on the skin that can become painful. They are caused by excessive pressure and friction on the skin. Corns press into the deeper layers of the skin and are usually round in shape.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as:
- Wearing properly fitting shoes that have been measured by a professional
- Wearing shoes that are not sharply pointed or have high heels
- Wearing only shoes that offer support
Treating Corns
Although most corns slowly disappear when the friction or pressure stops, this isn’t always the case. Consult with your podiatrist to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Everything You Need to Know About Corns
Corns are hard and thick areas of skin that form as a result of constant rubbing, friction, or pressure on the skin. They are patches of dead skin with a small plug toward the center. They may appear on the tops and sides of toes and can make walking painful.
Soft corns are typically thinner with a white color and rubbery texture. Soft corns tend to appear between the toes. Seed corns are another type of corn that appear in clusters and can be tender if they are on a weight-bearing part of the foot. Seed corns usually appear on the bottom of the foot and are likely caused by a blockage in sweat ducts.
While corns and calluses are somewhat similar, calluses are a bit different. Calluses are a patch of dead skin that can occur anywhere on the body. In comparison to corns, calluses are usually a bit larger in size. However, both corns and calluses are caused by increased friction on the skin.
There are some risk factors that may increase your chances of developing corns and calluses. If you have bunions, hammertoe, or a bone spur, you are more likely to develop a corn or callus on your foot.
While Corns and Calluses tend to disappear when the friction to the affected area ceases, the help of a podiatrist may be useful in the removal process. It is important to remove the dead skin around the area and this may be done in a few different ways. Moisturizing creams may be helpful in softening and removing the dead skin around the callus. You should never use razors or other pedicure equipment to remove your corns. Doing this may worsen your corn or callus and cause infection.
In some cases, corns and calluses may be caused by abnormal foot structure or walking motion. In such a case, you should seek a podiatrist’s assistance in order to correct the issue.
Who Needs an ABI Test?
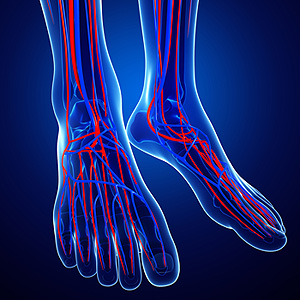 An Ankle-Brachial Index (ABI) test is a screening tool that is used to assess circulation in the lower limbs. During an ABI test, the doctor takes your blood pressure at various points along your arms and lower legs and compares the numbers to determine your risk of having full or partial blockages in the blood flow of your lower limbs. Not everyone needs an ABI test. They are typically done for people who are at risk of peripheral artery disease, a condition characterized by poor circulation in the extremities. People who are at risk of having peripheral artery disease include those with a history of smoking, high blood pressure, high cholesterol, diabetes, and atherosclerosis, as well as older adults and people who have a family history of peripheral artery disease. To learn more, please consult with a podiatrist.
An Ankle-Brachial Index (ABI) test is a screening tool that is used to assess circulation in the lower limbs. During an ABI test, the doctor takes your blood pressure at various points along your arms and lower legs and compares the numbers to determine your risk of having full or partial blockages in the blood flow of your lower limbs. Not everyone needs an ABI test. They are typically done for people who are at risk of peripheral artery disease, a condition characterized by poor circulation in the extremities. People who are at risk of having peripheral artery disease include those with a history of smoking, high blood pressure, high cholesterol, diabetes, and atherosclerosis, as well as older adults and people who have a family history of peripheral artery disease. To learn more, please consult with a podiatrist.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with Brian D. Jackson, DPM from Neuhaus Foot and Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
- Ankle-Brachial Index (ABI) examination
- Doppler examination
- Pedal pulses
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Vascular Testing in Podiatry
In foot care, vascular testing may be required in the diagnosing and treatment of certain podiatric conditions. Vascular testing is particularly relevant for patients with high-risk diabetes, poor circulation, peripheral artery disease (PAD), and chronic venous insufficiency (CVI). Procedures typically involve the examination of blood vessels throughout the body for blockages or buildup.
Vascular testing is very important for the diagnosis of various conditions, including peripheral artery disease and chronic venous insufficiency, as these conditions can greatly affect one’s quality of life and cause pain in the lower limbs. Circulatory problems in the feet and ankles can reflect issues throughout the body, making testing of the blood vessels pertinent.
Testing methods vary between practitioners and can be specific to certain foot and ankle problems. Modern technology has brought about the ability to perform vascular testing using non-invasive methods, such as the cuff-based PADnet testing device. This device records the Ankle-Brachial Index (ABI)/Toe-Brachial Index (TBI) values and Pulse Volume Recording (PVR) waveforms. Contact your podiatrist to determine what vascular testing is available for your needs.
What Causes Fallen Arches?
It is not uncommon for adults to experience a sudden onset of flat feet, known medically as posterior tibial tendon dysfunction (PTTD). The tibial tendon, which connects the calf muscles with bones on the inside of the foot, holds up the arch and supports the foot when you walk. This tendon can tear from playing sports like basketball, tennis or soccer, or become inflamed, causing the arch to fall. This injury is more common in women and adults over the age of 40. Other risk factors include obesity, diabetes and high blood pressure. Most fallen arches can be treated non-surgically with orthotics, shoes with good arch support, and braces. Sometimes a protective boot is worn to give the tendon a chance to heal properly. Treating PTTD early is highly recommended, as putting it off can lead to further complications, such as arthritis, that may impede your ability to walk, run, or take part in other physical activities. If you have noticed a sudden onset of flat feet, it is wise to make an appointment with a podiatrist as soon as possible for a full diagnosis and suggested treatment options.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Brian D. Jackson, DPM from Neuhaus Foot and Ankle. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flatfoot
Flatfoot is a foot disorder that is not as straightforward as many people believe. Various types of flatfoot exist, each with their own varying deformities and symptoms. The partial or total collapse of the arch, however, is a characteristic common to all types of flatfoot. Other signs of flatfoot include:
- “Toe drift,” or the pointing outward of the toes and the front part of the foot
- The tilting outward of the heel and the tilting inward of the ankle
- The lifting of the heel off the ground earlier when walking due to a tight Achilles tendon
- Hammertoes
- Bunions
One of the most common types of flatfoot is flexible flatfoot. This variation usually starts in childhood and progresses as one ages into adulthood. Flexible flatfoot presents as a foot that is flat when standing, or weight-bearing. When not standing, the arch returns. Symptoms of flexible flatfoot include:
- Pain located in the heel, arch, ankle, or along the outside of the foot
- Overpronation, or an ankle that rolls in
- Shin splint, or pain along the shin bone
- General foot aches or fatigue
- Pain located in the lower back, hip, or knee
Your podiatrist will most likely diagnose flatfoot by examining your feet when you stand and sit. X-rays may be taken to define the severity and help determine the treatment option best for your condition. Nonsurgical treatments can include activity modification, weight loss, orthotics, immobilization, medications, physical therapy, shoe modifications, and ankle foot orthoses (AFO) devices. If nonsurgical methods prove ineffective, surgery may be considered. Multiple surgical procedures can correct flatfoot; and depending on your specific condition, one may be selected alone or combined with other techniques to ensure optimal results.
The Importance of Treating Foot Wounds
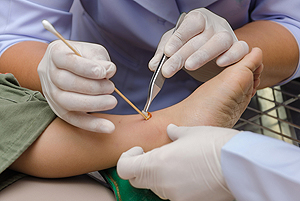 When the outer layers of the skin on the feet are damaged and expose deeper tissues, it is known as a foot wound or ulcer. These wounds can occur from issues such as wearing shoes that don’t fit correctly, as well as an injury or trauma to the feet. If these wounds are left untreated, they may become infected which could lead to other issues including amputation. Common indicators of an infection include inflammation, redness, an odor, or thickened tissues. Patients who are at a higher risk for foot wounds (such as diabetics, who may have trouble feeling the wounds) or who notice that their foot wound is not healing, should have the wound looked at by a podiatrist. Upon examination, a podiatrist will likely remove the unhealthy skin and then help determine the best treatment method for the particular wound, including shoe padding, antibiotics, or even surgery.
When the outer layers of the skin on the feet are damaged and expose deeper tissues, it is known as a foot wound or ulcer. These wounds can occur from issues such as wearing shoes that don’t fit correctly, as well as an injury or trauma to the feet. If these wounds are left untreated, they may become infected which could lead to other issues including amputation. Common indicators of an infection include inflammation, redness, an odor, or thickened tissues. Patients who are at a higher risk for foot wounds (such as diabetics, who may have trouble feeling the wounds) or who notice that their foot wound is not healing, should have the wound looked at by a podiatrist. Upon examination, a podiatrist will likely remove the unhealthy skin and then help determine the best treatment method for the particular wound, including shoe padding, antibiotics, or even surgery.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Brian D. Jackson, DPM from Neuhaus Foot and Ankle. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact one of our offices located in Columbia and Pulaski, TN . We offer the newest diagnostic and treatment technologies for all your foot care needs.